Researchers at the RIKEN Center for Sustainable Research Science (CSRS) and the University of Toronto have discovered a new way to attack fungal infections. The key is to block fungi from being able to make fatty acids, the major component of fats. Resistance to anti-fungal drugs is increasing and this new approach will be particularly useful because it works in a new way and affects a broad range of fungal species. The study was published in the scientific journal Cell Chemical Biology.
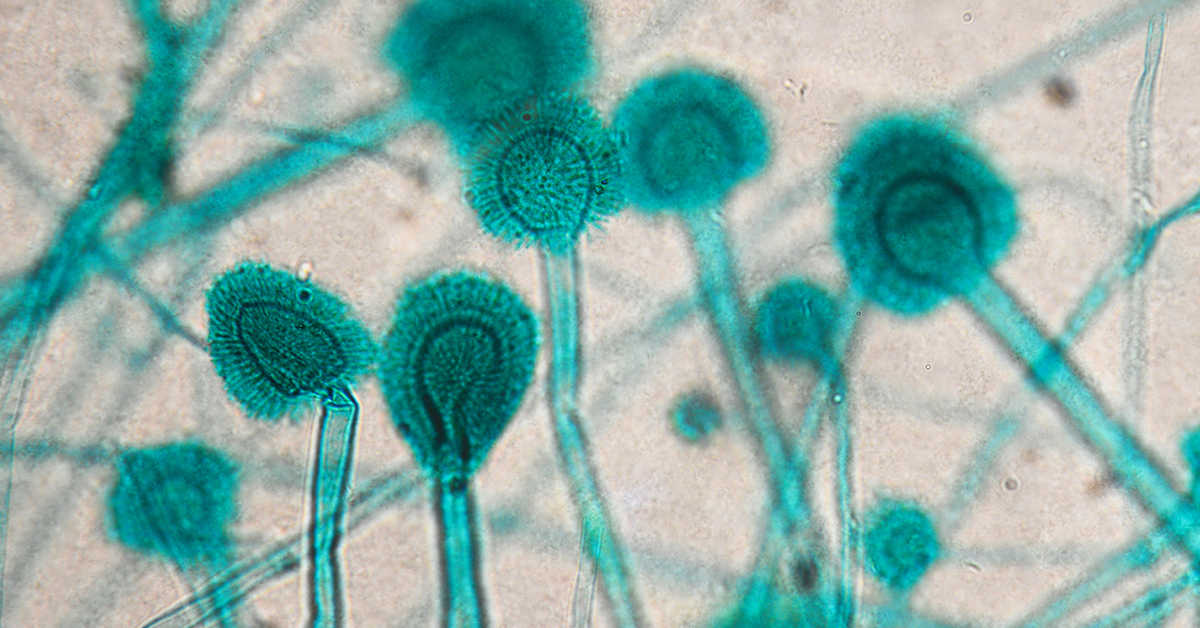
Most of us are familiar with athlete’s foot, a relatively harmless health issue that can be solved by a trip to the drug store. But other fungal infections are more serious, and the Candida, Cryptococcus, and Aspergillus types of fungus are responsible for millions of deaths every year. Like bacterial resistance to antibiotics, fungal resistance to medications is also growing worldwide, and the death toll will likely rise in the near future unless something is done now.
Currently there are only three major classes of anti-fungal medications, and all of them work by destroying the barrier that surrounds fungal cells. Paradoxically, even though they all attack the barrier, current treatments are actually very specific, meaning that what kills one species of fungus might not kill another.
The group of researchers wanted to find another way to combat harmful fungi, one that would be useful against numerous species. Their approach was to first screen the structurally-diverse RIKEN natural product depository (NPDepo) against four pathogenic yeasts—three Candida and one Cryptococcus species—which have been identified as critical human pathogens by the World Health Organization. They were looking for something that would affect all four species, which would indicate that it might be effective against a broad range of fungi.
The screening identified several compounds that reduced fungal growth by at least 50% in each of the four species, and after eliminating ones which were already known, the researchers were left with three new possibilities. Among these three, the one least toxic to human cells also reduced growth of Aspergillus fumigatus, an extremely common fungal mold that is deadly to immuno-compromised individuals. The name given to this compound in the RIKEN NPDepo is NPD6433. The next step was to find out what it does.
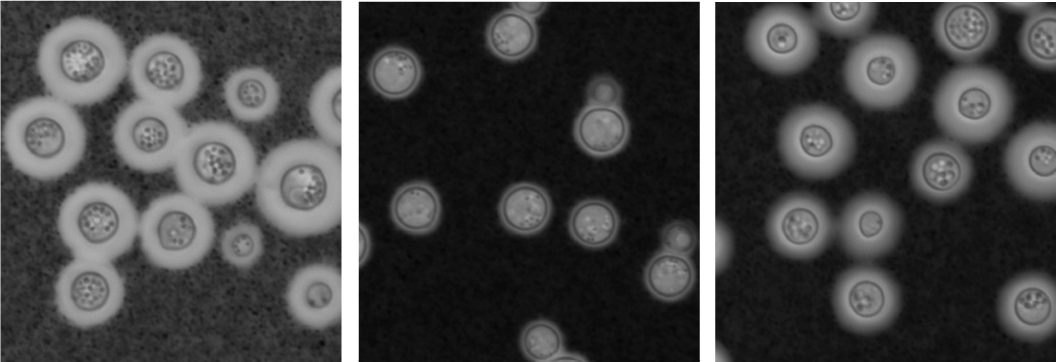
The virulence of fungi was reduced with sub-lethal doses of NPD6433. (Left) Untreated C. neoformans (yeast) grown in culture. (Middle) C. neoformans treated with NPD6433. (Right). C. neoformans treated with fluconazole, a drug used to treat serious yeast infections. By staining the slides with India ink, we can see that capule size, a sign of virulence, is greatly reduced with NPD6433, but only slightly reduced with fluconazole. The number of yeast was also reduced more with NPD6433.
For almost 1000 different genes, the researchers looked at how much NPD6433 suppressed growth in yeast when the yeast was missing one copy of the gene. They found that reduction in only one gene, fatty acid synthase, made yeast more susceptible to NPD6433. This result meant that NPD6433 likely works by inhibiting fatty acid synthase and thus prevents fatty acids from being made inside fungal cells. Further experiments showed that NPD6433 and cerulenin, another fatty acid synthase inhibitor, were able to kill numerous yeast species in culture.
The final experiment tested how well NPD6433 treatment worked in a live laboratory model organism—the worm Caenorhabditis elegans—which was infected with a pathogenic yeast that can cause systemic infection in humans after invading through the intestines. C. elegans was chosen because it has an intestinal tract that works like ours. Tests showed that treating infected worms with NPD6433 reduced fatalities by about 50%. Importantly, this was true in worms infected with yeast that were resistant to a standard anti-fungal medication.
“Drug-resistant fungi are a growing problem, and leads for the development of new drugs offer hope against these evolving pathogens,” says Yoko Yashiroda, lead RIKEN CSRS author of the study. “Our research indicates that targeting fatty acid synthesis is a promising alternative therapeutic strategy for fungal infections, and one which might not require tailor-made solutions for individual species.”
Most of us are familiar with athlete’s foot, a relatively harmless health issue that can be solved by a trip to the drug store. But other fungal infections are more serious, and the Candida, Cryptococcus, and Aspergillus types of fungus are responsible for millions of deaths every year. Like bacterial resistance to antibiotics, fungal resistance to medications is also growing worldwide, and the death toll will likely rise in the near future unless something is done now.
Currently there are only three major classes of anti-fungal medications, and all of them work by destroying the barrier that surrounds fungal cells. Paradoxically, even though they all attack the barrier, current treatments are actually very specific, meaning that what kills one species of fungus might not kill another.
The group of researchers wanted to find another way to combat harmful fungi, one that would be useful against numerous species. Their approach was to first screen the structurally-diverse RIKEN natural product depository (NPDepo) against four pathogenic yeasts—three Candida and one Cryptococcus species—which have been identified as critical human pathogens by the World Health Organization. They were looking for something that would affect all four species, which would indicate that it might be effective against a broad range of fungi.
The screening identified several compounds that reduced fungal growth by at least 50% in each of the four species, and after eliminating ones which were already known, the researchers were left with three new possibilities. Among these three, the one least toxic to human cells also reduced growth of Aspergillus fumigatus, an extremely common fungal mold that is deadly to immuno-compromised individuals. The name given to this compound in the RIKEN NPDepo is NPD6433. The next step was to find out what it does.
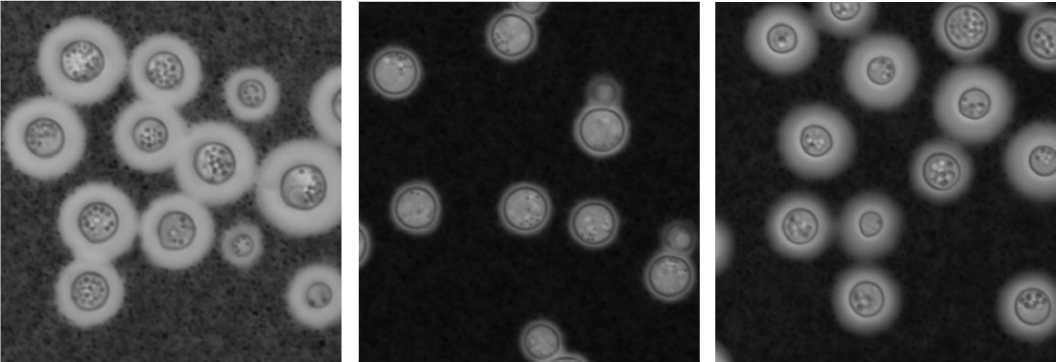
The virulence of fungi was reduced with sub-lethal doses of NPD6433. (Left) Untreated C. neoformans (yeast) grown in culture. (Middle) C. neoformans treated with NPD6433. (Right). C. neoformans treated with fluconazole, a drug used to treat serious yeast infections. By staining the slides with India ink, we can see that capule size, a sign of virulence, is greatly reduced with NPD6433, but only slightly reduced with fluconazole. The number of yeast was also reduced more with NPD6433.
For almost 1000 different genes, the researchers looked at how much NPD6433 suppressed growth in yeast when the yeast was missing one copy of the gene. They found that reduction in only one gene, fatty acid synthase, made yeast more susceptible to NPD6433. This result meant that NPD6433 likely works by inhibiting fatty acid synthase and thus prevents fatty acids from being made inside fungal cells. Further experiments showed that NPD6433 and cerulenin, another fatty acid synthase inhibitor, were able to kill numerous yeast species in culture.
The final experiment tested how well NPD6433 treatment worked in a live laboratory model organism—the worm Caenorhabditis elegans—which was infected with a pathogenic yeast that can cause systemic infection in humans after invading through the intestines. C. elegans was chosen because it has an intestinal tract that works like ours. Tests showed that treating infected worms with NPD6433 reduced fatalities by about 50%. Importantly, this was true in worms infected with yeast that were resistant to a standard anti-fungal medication.
“Drug-resistant fungi are a growing problem, and leads for the development of new drugs offer hope against these evolving pathogens,” says Yoko Yashiroda, lead RIKEN CSRS author of the study. “Our research indicates that targeting fatty acid synthesis is a promising alternative therapeutic strategy for fungal infections, and one which might not require tailor-made solutions for individual species.”
Further reading
Iyer et al. (2023) Identification of triazenyl indoles as inhibitors of fungal fatty acid biosynthesis with broad-spectrum activity. Cell Chemical Biology. doi:10.1016/j.chembiol.2023.06.005
Further reading
Iyer et al. (2023) Identification of triazenyl indoles as inhibitors of fungal fatty acid biosynthesis with broad-spectrum activity. Cell Chemical Biology. doi:10.1016/j.chembiol.2023.06.005